
iPS細胞×角膜移植で拓く未来の光
世界的な高齢化の中、増えゆく眼疾患「水疱性角膜症」。
治療法は角膜移植のみ、だが待機患者も増えるばかり――。
この状況に対し、iPS細胞を用いた独自の治療法を開発し、社会実装を目指す再生医療ベンチャー、セルージョン。
慶應義塾大学医学部発、革新的な治療技術に邁進する研究者の想いから、未来を変える一筋の光が見えてくる。
「水疱性角膜症」を巡る、角膜移植と移植待機患者の問題
弊社は失明につながる目の病気「水疱性角膜症」に対して、iPS細胞を用いた新たな治療法を確立するため、2015年に設立された慶應義塾大学医学部発のベンチャー企業です。水疱性角膜症とは、角膜の内皮細胞が厚く濁った状態になる疾患で、その多くは白内障手術後の合併症によって角膜の内皮細胞がダメージを受けることに起因します。白内障手術は非常にポピュラーな手術であり、水疱性角膜症の発症率はそのうちごくわずかに過ぎませんが、世界的な高齢化とともに白内障手術の施術数が今後増えていく以上、水疱性角膜症の患者数もまた、増加の一途を辿ることは避けられません。
そして、この水疱性角膜症に有効な治療法が角膜移植です。現在行われている角膜移植のうち、水疱性角膜症の患者数は50パーセント以上に上ります。しかし、角膜移植には以下の3つの問題があります。まず、角膜移植にはドナー眼(提供者の眼球)が必要なこと。手術には高度な技術が求められ、専門の医師と手術設備が必要になること。さらに、ドナーの眼球を適切に患者に分配するための社会システムとして、「アイバンク」制度が整っていることも欠かせません。これらの条件を満たしているのは、世界でも先進国を中心とする地域に限定されます。現状、全世界で1270万人以上と報告される角膜移植の待機患者のうち、移植手術の実施数は年間18万件に過ぎません。ここに、角膜移植を取り巻く大きな社会問題があります。
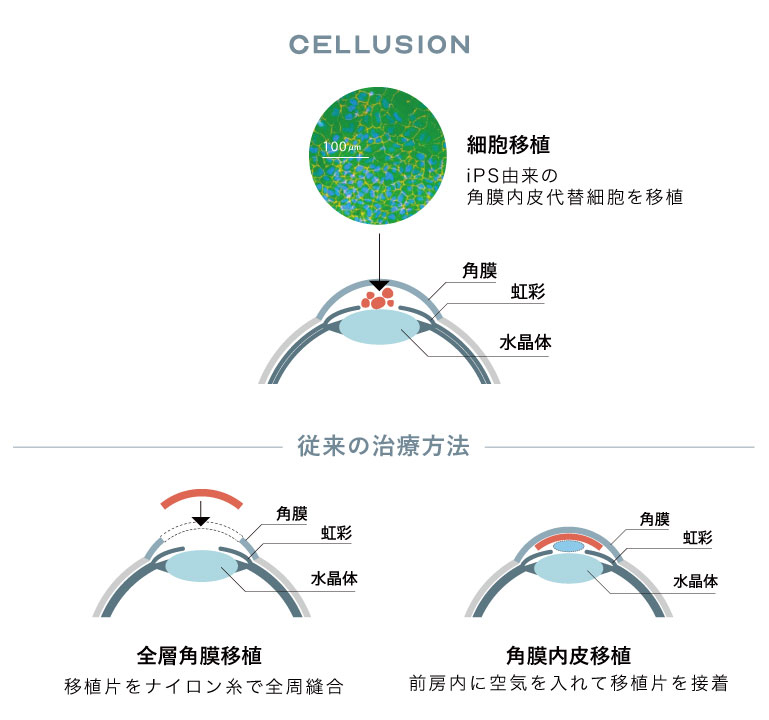
しかし私たちはこの問題を、iPS細胞を用いた再生医療で解決できると考えています。具体的には、iPS細胞を使って角膜内皮の代替細胞を製造し、その細胞を目に移植する。手術は細胞をシリンジ(注射器)で注入するだけで、細胞は術後3時間、うつ伏せの姿勢を維持すれば重力によって角膜へと定着します。この治療法であれば先の3つの条件に対し、iPS細胞によって角膜内皮細胞の大量生産ができ、角膜移植の専門医や専門施設の必要がなく、クリニックでも治療が可能になる。ドナーの眼球が必要なく、アイバンクシステムも不要なため、世界中で実施することができるようになるでしょう。
iPS細胞による治療法確立のため、医学部発ベンチャーを設立
私は角膜移植専門の眼科医として、この画期的な治療法を慶應義塾大学医学部眼科学教室の坪田一男教授、榛村(しんむら)重人准教授とともに研究してきました。患者の目に細胞をシリンジで注入し、角膜内皮細胞へ定着させる手術方法自体は、京都府立医科大学など先行するグループの研究の中で生み出されてきた方法ですが、私たちの場合はドナー眼から採取した内皮細胞ではなく、iPS細胞由来の代替細胞を使う点がポイントです。研究を通してこの治療法の有効性を確信する一方で、次第にアカデミアの力だけでは社会実装を達成できないと考えるようになり、15年にセルージョンを設立しました。
しかし、設立当初は本当に苦労の連続でした。当時は慶應義塾大学医学部の教員によるスタートアップの前例がほとんどなく、教育機関としてこうした試みをどうやってマネジメントしていくか、大学側でも体制の整備が必要だったのです。私たちもまた、iPS細胞技術の事業化促進に取り組む株式会社iPSポータルを株主に迎え、その支援を得ながら手探りで会社運営のあり方を固めていく中で、KIIを紹介していただきました。それが17年12月のこと。以来、KIIには資金面だけでなく、スタッフの方が社外取締役として加わるなど、組織面や会社運営までをサポートしていただいています。
幸い我々は大学からの研究資金によって、最初の細胞製造プロセスから非臨床の動物実験の初期段階へと到達することができました。しかし、続いて必要な安全性試験や動物実験、最終的な患者様への投与を伴う臨床研究を進めるにあたり、今後さらなる資金調達が必要になります。また、資金面、技術面とは別の課題として国の制度をクリアする必要もあります。何より重要なのは、この治療技術を全世界の眼科医が使えるようにディストリビューションしていくこと。そのためには、細胞を安定して大量生産するための製造技術や保存方法を確立しなければなりません。専門医でなくとも使いやすい剤型や凍結保存方法、輸送方法まで……。これらは論文の対象にはならない領域ですが、その知見をいち早く製造方法に組み込むことで、より迅速な開発を心がけるようにしています。

“研究者×眼科医”の発想を原動力に、世界の幸せに貢献する
こうした開発のあり方には、私がこれまでに経験してきた、“研究者と眼科医”という二つの要素が影響しているかもしれません。「もし自分が開業医だとしたら、どんなものであれば使いたいと思うだろう?」という発想を常にキープしておき、研究開発にも活かしていく。幾ら効果のある治療法でも、1回あたり何百万円もコストがかかったり、大がかりな設備が必要だったりするものは、決して導入しやすいとは言えません。世界中の医師たちに使ってもらえるような治療法にするためには、できるだけ大量生産ができて、クリニックでも導入できる販売価格を実現する必要があります。
そして開発に取り組むモチベーションとしては、社会的な問題を解決したいという想い、これに尽きると思います。科学の研究は、実験を100回実施して1パーセントの可能性を見いだせるか否かという、非常に地道で厳しい世界です。それでも社会的な使命感を忘れることなく、一歩前進できた時の手応えがあるからこそ、「これをやり遂げたい」と信じ続けることができるのだと思います。私自身の話をするなら、慶應義塾大学医学部を卒業後に一般消化器外科と小児外科を経て眼科医になり、恩師の声がけで国立病院機構 東京医療センターにて角膜移植の研究を始め、慶應義塾へと戻ってきたという、医師としては変わったキャリアパスを辿ってきました。その中で培ってきた“研究者と医師”という二つの側面が、大学病院の勤務医や開業医と比べて大きなリスクを取ってでも、新しいことを目指す気持ちにつながっていると感じます。
水疱性角膜症には、角膜移植という治療法はあるものの、世界中に非常に多くの待機患者が存在しており、その数は今後どんどん増えていく。この問題を新たな治療法によって解決した暁には、さらに新たな疾患にも取り組みたいと考えています。角膜移植が必要な疾患のうち、水疱性角膜症以外の約40パーセントにあたる角膜実質や角膜上皮の疾患にも、再生医療による治療法を広げていきたい。
人間にとって目の病気は、幸せな人生を営んでいくためのQOL(クオリティ・オブ・ライフ)に大きく関わる問題です。新たな治療技術によって、世界中の人々の幸せに貢献したい。その想いが、私たちの大きな原動力になっています。
【公式サイトへのリンク】
https://cellusion.jp/